Jeremy Wilson and Roy Fenoff, 2009

Counterfeit Pharmaceuticals
Counterfeiting, perhaps one of the oldest and most profitable occupations, can be traced back to the times of the ancient Egyptians and early Greeks (Penn, 1979). Advancements in technology have facilitated the production and distribution of larger quantities of counterfeited goods in shorter periods of time, and have made it easier for counterfeiters to profit while successfully escaping detection. The FBI calls counterfeiting the crime of the 21st century (United Nations Interregional Crime and Justice Research Institute, 2003) and the trafficking of counterfeit goods has become one of the world’s largest and most rapidly growing criminal enterprises, with the International AntiCounterfeiting Coalition (IACC) estimating a value of more than US$ 600 billion annually (IACC, 2009). Today, counterfeit goods are found throughout the world; wherever there is a demand for a product, counterfeiters are quick to fill the niche. The kinds of counterfeited products identified by the Organization for Economic Cooperation and Development (OECD) include clothing, auto parts, money, electronics, food, water, and pharmaceuticals (OECD, 2007).
The damage caused to society by counterfeit goods varies in scope and scale depending on the product and its range of distribution. However, of all the different counterfeit goods produced, none are more potentially damaging than those affecting public health and safety, such as pharmaceuticals. The World Health Organization (WHO) estimates that of the 1 million malaria deaths that occur each year, 200,000 are the result of counterfeit anti-malarial drugs (WHO, 2003). Harris, Stevens, and Morris (2009) state that counterfeit drugs for tuberculosis and malaria kill 700,000 people every year. Although the counterfeit drug trade is wide in scope, it has a more devastating public health effect on developing countries, like those in Southeast Asia and Africa, where there are intense demands for inexpensive lifesaving drugs. This paper presents an overview of the current knowledge of the counterfeit drug trade in Africa, with the aim to generate discussion about the necessary steps to understand and respond to this problem.
Before discussing counterfeit drugs, it is necessary to define the term. Because the extent of the problem differs from country to country, the concept of “counterfeit drug” varies. For the purpose of this paper we will use the definition developed by the WHO (2009):
A counterfeit medicine (drug) is one which is deliberately and fraudulently mislabeled with respect to identity and/or source. Counterfeiting can apply to both branded and generic products and counterfeit products may include products with the correct ingredients or with the wrong ingredients, without active ingredients, with insufficient active ingredients or with fake packaging.
The Magnitude of Counterfeiting is Significant
Traditionally, the most common types of counterfeit drugs were those described as “lifestyle drugs” such as those used to treat erectile dysfunction or baldness. However, recently there has been an increase in the counterfeiting of “lifesaving” drugs meant to prevent or treat asthma, malaria, cancer, HIV/AIDS, tuberculosis, blood pressure and heart conditions, diabetes, and severe diarrhea. In Africa, the three forms of drugs most frequently counterfeited are those aimed at malaria, HIV/AIDS, and tuberculosis (Amin & Kokwaro, 2007; Kapp, 2002).
The counterfeit drug epidemic currently threatening many African countries is gaining international attention. World leaders are beginning to realize that the counterfeit drug trade is not a local problem faced by a few developing countries, but a global one with far-reaching consequences. Surprisingly, even with an estimated US$ 39 billion annual world market (Pitts, 2005), little is known about its geographic extent. Organizations such as the UN, the WHO, the World Trade Organization, and the OECD, and some government agencies, such as Nigeria’s National Agency for Food and Drug Administration and Control (NAFDAC), have collected some startling statistics over the past few years. Armed with these data and following some high-profile arrests, these organizations have made public the impact of the counterfeit drug epidemic in developing countries and the steps that leaders are taking to bring the counterfeiting problem under control.
According to the WHO, a significant fraction of the world’s drug supply is counterfeit. Estimates of counterfeit drugs range from 10 to 15 percent for the world drug supply, to more than 30 percent of all medicine sold in Africa, and up to 70 percent of the drugs sold in Nigeria WHO, 2008; Primo-Carpenter, 2009). In 2005 the estimated US$ 39 billion global market for counterfeit drugs was growing at 13 percent annually, with a projected increase of 92 percent to reach US$ 75 billion by 2010 (Pitts, 2005). It is important to acknowledge, however, the difficulty of measuring the extent of counterfeiting with any degree of certainty. The clandestine nature of much of the manufacture, distribution, and sale of counterfeits make creating an appropriate sampling frame challenging, thereby inhibiting the accuracy of prevalence estimates. It is difficult to assess how well the sample drawn to test for counterfeits represents the true population of pharmaceuticals in the market.
Because so little is known about the counterfeit drug trade in Africa it is difficult to provide any solid information regarding regional differences. Much of the published information is “recycled” in that organizations often cite each others’ statistics. Most of the information has been collected by international organizations and local government personnel and there are few empirical studies. Even with limitations, it is certain that the trade of counterfeit drugs is thriving throughout Africa, and most countries have been unable to effectively combat the threat.
A Model of the Counterfeiting Process
The process of creating counterfeit drugs is similar to counterfeiting any other product and the goal is the same: fabricate false product and/or false labels. Some drugs are produced with no, little, or too much active ingredient while others are composed (intentionally or otherwise) of toxic substances (Bate, 2008a). Other methods include forging labels by changing expiration dates, packaging information, holograms, or trademarks (Forzley, 2003; Sukhlecha, 2007). The imitation or altered product is then produced in various quantities and entered into a need-driven market in which large profits are often made.
Because the trade in counterfeit drugs usually uses complex distribution networks, researchers have been unable to create a distinct criminal profile that identifies counterfeit drug producers and sellers. However, to combat the trade it is necessary to understand how counterfeit drugs are introduced into the distribution system. Figure 1 illustrates a three-component counterfeiting process: supply, process, and demand. The model, based on open source documentation, describes how the practice works and identifies areas of opportunities for counterfeiters to enter drugs into the African market.
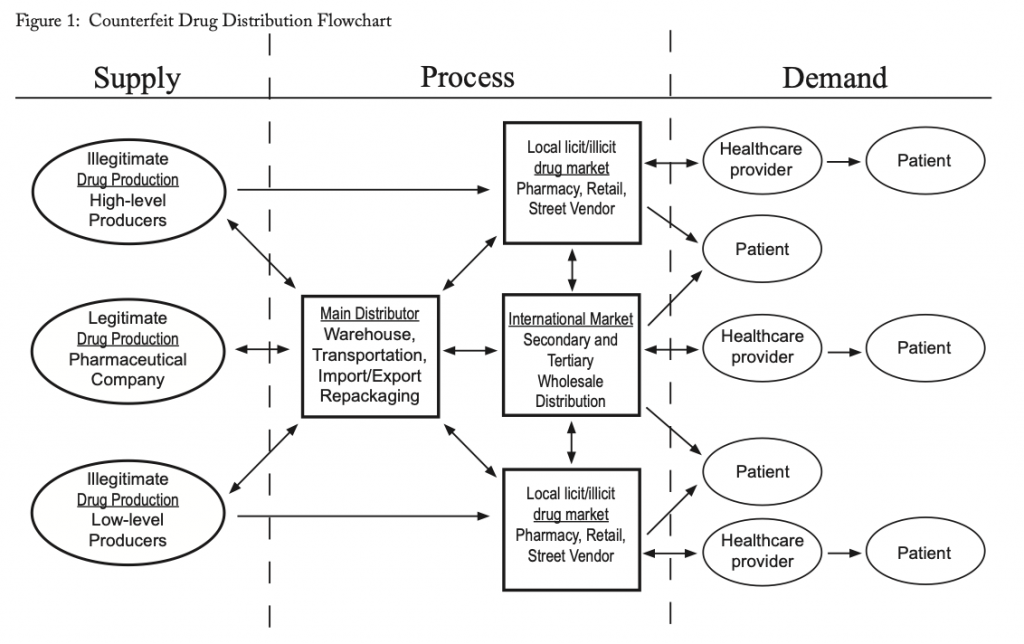
As shown in this model, it is not a single pathway from the manufacturer to the distributor to the customer (for additional depictions of the pharmaceutical supply chain, see Kontnik, 2004; OECD, 2008; Yankus, 2006). The arrows indicate points in the supply chain where drugs exchange hands—each such instance is an opportunity for illegal activity. The process relies on a wholesale distribution network which often includes numerous distributors, intermediaries, and secondary and tertiary wholesalers. Although this process is multifaceted and often may seem confusing, it actually makes the delivery of drugs more efficient and economical for the supplier (Eban, 2006). The process allows the supplier to produce drugs in large quantities and then sell them in lots to distributors, who then pass the products along the distribution network where small wholesalers are able to quickly find buyers. The distribution network is a mix of legitimate, semi-legitimate, and criminal players (Phillips, 2007). As a result, the wholesale market opens the door for counterfeits and substandard drugs to be introduced into the supply chain (Patton, 2007). One way this is accomplished is through diversion, or the manipulation of the legal flow of drugs. This can result in the authentic product being sold outside the intended market while creating an opportunity to introduce fakes into the supply chain. The USFDA claims that every case of counterfeiting is followed by diversion (Daleiden, 2009).
As outlined in the model, the process begins with the manufacturer, who can be a legitimate pharmaceutical company or an illegitimate high- or low-level producer.The producers may directly enter the product into the local licit or illicit market or they may pass it on to a distributor who is often connected to a criminal network (Kontnik, 2004). The distributor may then directly enter the product into the local licit or illicit market or sell the counterfeit drugs to wholesalers in the international market. These secondary wholesalers may then pass the product on to the local licit and illicit markets, or pass it on to a tertiary wholesaler who continues to forward the drugs along the supply chain; in some cases they may even sell the drugs directly to patients or healthcare providers (Kontnik, 2004).
The process also works in reverse. Drugs that are damaged or expired are returned to the producer for destruction. However, many of these drugs never make it back to the manufacturer but are instead diverted, repackaged and or relabeled, and then inserted back into the supply chain to be resold to consumers (Yankus, 2006).
It has also been claimed that the high-level producers are the ones who sell the counterfeit drugs to criminal networks; some of these producers have been linked to terrorist groups (Bate 2008a; International AntiCounterfeiting Coalition, 2005). INTERPOL has identified a relationship between counterfeit drugs and terrorist financing; the relationship is either direct, when a terrorist group produces and sells the goods, or indirect, when the group receives funds from sympathizers (INTERPOL, 2009).
The internet expands opportunities for these diverse groups to connect. It is well known that Africa is becoming a hot spot for Internet scams; some of the better known frauds include phishing scams and the Nigerian 419 scam (BBC News, 2003; Namibia Economist, 2009). With an increasing number of Africans using the Internet, the number of cybercrimes continues to grow (Wanjiku, 2009). It is reasonable to expect these trends to exacerbate the counterfeiting problem in African countries.
Supplier Characteristics are Largely Unknown

Those who take part in the production and distribution of counterfeit pharmaceuticals are extremely diverse (e.g., in terms of role, extent of involvement, and level of organization) and hard to identify, as the flow of these drugs involves numerous people and organizations from different parts of the world. Criminals include individuals, pharmacists, doctors, criminal groups, pharmaceutical companies, corrupt government officials, and terrorist organizations (OECD, 2008). Established organized crime groups such as the Russian mafia (OECD, 2008) and Chinese triads (Kafchinski, 2009) are thought to be one of the main players in the lucrative business of counterfeit drugs (Lybecker, 2008). In fact, there have been reports both of drug cartel leaders switching from trafficking in illegal drugs of abuse like cocaine to counterfeit pharmaceuticals (Yankus, 2006) and of cartel leaders adding counterfeiting to their business plans (Patton, 2007). While both activities are profitable, the punishment for counterfeiting is relatively minor, with the most common penalty being a fine, while a conviction for dealing cocaine can lead to life imprisonment. Although it is not readily apparent who and how people behind the transportation and distribution of these drugs are organized, the drug origins are more clear. Roger Bate (2008a), a director of the NGO Africa Fighting Malaria states:
Nearly every observer and researcher on (the) hunt for these dangerous fakes will point to two primary culprits: China and India. My own research on antimalarial drugs suggests that 60 to 80 percent of those fake drugs come from these two countries alone.
Peter Pitts (2005), president of the Center for Medicine in Public Interest, agrees with Bate and testified before the US Senate that China plays a central role in counterfeit drug production, with over 50 percent of the global supply of counterfeit pharmaceuticals having Chinese origin. Recently, Chinese Ambassador to Nigeria, Rong Yansong, issued a formal apology for the counterfeit drugs that have entered Nigeria from China and explained that the Chinese government would ensure the punishment of fake drug exporters (Nwezeh, 2009).
Nigeria: Drug Agency Raises Alarm Over Illegal Act of Fake Drugs in Kano State
June 22, 2009 Lagos The Guardian Online
An alarm was at the weekend raised by the National Agency for Food and Drug Administration and Control (NAFDAC) that Kano has assumed the position of a sanctuary where manufacturers of fake food and drugs carry out their heinous activities. The agency’s Director of Enforcement, Mr. Hashim Ubale Yusufu, made this known yesterday at a press briefing at the Kano chapter of the Nigeria Union of Journalists (NUJ) secretariat. Reading the Riot Act to distributors, wholesalers, and retailers of pharmaceutical and other NAFDAC-regulated products to stay away from such illegal act; he disclosed that a survey conducted by NAFDAC’s officials indicates that counterfeiting activities is shifting from Onitsha and Lagos to Kano.
Yusufu…disclosed the discovery of a warehouse beside Kwari market fully stocked with counterfeit regulated drugs comprising 142 cartons of Tramadol capsules, 574 cartons of Ibumol as DA-ibugold, 244 cartons of chloraphenicol eye drop and packs of Tarivid tablets. He also disclosed the arrest of an illegal manufacturer, who was caught with large quantity of unpacked baking powder called ‘Super Baking Powder’ as well as large quantities of fake curry powder known as ‘Duros’ at 2A Sansus Street, Sabongari, Kano. He further disclosed the discovery of a warehouse at Unity Road stocked with over 1300 cartons of Husna Kajal made in Pakistan, 118 cartons each containing 12 dozens of ‘kalakola hair colour,’ 24 cartons of different unregistered bleaching creams, which had no manufacturers’ name, address, batch number, manufacturing date, expiry date and list of ingredients on the packaging materials or labels.
A Distribution Process with Criminal Opportunity
African countries are attractive targets for trade in counterfeit pharmaceuticals; numerous factors allow criminal organizations to make enormous amounts of money with little risk of being caught. One is the extremely high level of poverty and disease across the continent. According to the WHO, laws and levies added 69 percent to the cost of legitimate drugs in 2003, making it impossible for most Africans to afford medicines from legal sources and further driving illicit drug markets (Bale, 2001). Harris et al. support this contention, arguing that government-imposed distortions of the medicines market through taxes, tariffs, price controls, and licensing regimes contribute to the counterfeit drug epidemic. At least 103 pharmacies in South Africa have closed due to price caps on pharmaceuticals (Tren, 2005). A second factor is the ease with which smugglers are able to get their products into different African countries. Harris et al. (2009) explain that the often flawed legal systems of developing countries contribute to this process. The countries also generally lack the necessary resources to invest in technologies to test and identify counterfeit drugs. One of the most common techniques to evade detection is to disguise counterfeit drugs as legal imports, by changing the appearance of the items, providing fraudulent documentation with forged signatures, or both. The number of corrupt and/ or politicized legal systems in which informal payments can be easily made in order to pass counterfeits through bureaucratic barriers facilitate this fraud; some contend that many customs agents and police officers are easily bribed or fooled by forged documents (Harris et al., 2009; Anonymous, 2008; Buyonge & Kireeva, 2008; Edmonson, 2005; Beisecker, 2005). More sophisticated criminals use small amounts of the drug’s active ingredient, referred to as “salting”, so when and if a drug is tested it passes as the real product (Mukhopadhyay, 2007). Smugglers will also conceal counterfeit drugs within legal shipments or use common delivery systems.
The Increasing Demand for Inexpensive Lifesaving Drugs
Like many other illicit markets such as the illegal trade of wildlife, weapons, and human trafficking, the trade of counterfeit drugs is a lucrative business with a growing demand that continues to fuel the trade. However, unlike the illegal trade of wildlife, weapons, and humans, which tend to have a demand driven by wealthier countries (World Wildlife Fund, 2002; Pitts, 2005), the demand for counterfeit drugs is highest in impoverished, less developed countries (Khan & Ghilzai, 2007; Harris et al., 2009; Taylor, 2008). These nations face problems that the developed world is able to escape. For instance, infectious diseases are prevalent across the African continent and a majority of the population is unable to afford or obtain access to lifesaving drugs through legitimate channels (Bate, 2008b; Bale, 2001). As a result, many African countries have been bombarded with counterfeit drugs and the governments have had little success in preventing these products from reaching local markets. According to Dr. Taryn Vian (2006), a healthcare expert from Boston University, the market for drugs in the developing world continues to grow with the rate of HIV/AIDS. This increased demand for cheap drugs has resulted in an influx of counterfeits entering the private and public markets in countries whose government regulatory systems are ineffective (Harris et al., 2009). The groups most affected by this are the poor and vulnerable populations (Harris et al., 2009; Vian, 2006).
The Nigerian Menigitis Epidemic, World Health Organization 2003
In 1995, a meningitis epidemic broke out in Niger. In response to the crisis, Niger authorities organized a country wide vaccination campaign. In an effort to combat the outbreak, Nigeria donated 88,000 vaccines which were given to more than 60,000 people. After the vaccines were administered, more than 25,000 people died. The Niger authorities suspected that the donated vaccines may have caused the deaths and conducted an investigation. The findings confirmed their suspicions that the drugs supplied had been substituted with counterfeit drugs that contained no active ingredients.
Counterfeit Drugs Have Devastating Impacts on Health and Economies
According to INTERPOL, malaria, tuberculosis, and HIV/AIDS are responsible for the deaths of more than 6 million people a year (Selgelid, 2007). Overall, P. falciparum malaria kills more than 900,000 Africans annually, mostly children under 5 years old (Centers for Disease Control, 2009). It is also estimated that 200,000 children die each year after taking counterfeit anti-malarial medications (INTERPOL, 2008a). When the total deaths from malaria and tuberculosis are combined, the estimated number of deaths attributed to counterfeit drugs rises to 700,000 annually (Harris et al., 2009). Although this is an alarming number in itself some researchers claim it is actually a conservative estimate (Harris et al., 2009). Empirical studies in bacteria and parasite drug resistance and tests of active ingredient levels in counterfeit drugs have been conducted. A recent study published in The Lancet concluded that up to 40 percent of products labeled as containing the anti-malarial agent artesunate contained no active ingredients (WHO, 2006a). A random survey in Kenya found that almost 30 percent of the all drugs were counterfeit, with some drugs being no more than chalk or water (WHO, 2006b). Another study analyzed 195 packs of anti-malarials that were sold in six African countries and found that 35 percent of them did not contain efficacious levels of active ingredients (Bate, Coticelli, Tren, & Attaran, 2008). The danger of receiving drugs with inadequate levels of active ingredient is two-fold. First, the individuals receive no therapeutic value from the drug, which increases their risk of death, and secondly, the low levels of active ingredient assist the microorganisms in adapting to the drugs making the drugs less effective. Regarding the drug resistance of the malaria parasite (Plasmodium), malaria expert Dr. Nick White of Oxford University said the following,
Counterfeit medicine is a major reason why malaria had become, over the past 30 years Africa’s biggest child killer, from an illness that used to be easily treated with medicines. There is now just one family of drugs left that malaria has not built up resistance to, Artemisinins – which are being faked….Resistance to the Artemisinins would be an absolute catastrophe for our current attempts to try to control malaria (Shah, 2007).
In addition to the devastating effects of drug resistance, counterfeit drugs also harm businesses and local economies. Counterfeit drugs affect companies that are producing genuine products because the counterfeit products will undersell the real ones. For example, an anti-malarial in Kenya that sells for $5 a dose is competing with counterfeits that are sold for $1 a dose (BBC News, 2007). Because it is an illegal trade, the counterfeiters do not pay any import duties when they bring the drugs into the country and they do not pay any sales tax on the drugs that they sell so the local economy also suffers.
The DRC: Health Ministry Warns Citizens Against Counterfeit Anti-Malaria Drug
June 12, 2009 Dakar PANA Online
Kinshasa, DR Congo (PANA) – The Health Ministry of the Democratic Republic of Congo (DRC) has warned citizens against the purchase of “Quinizen 20%” drug, said to be counterfeit quinine, a government statement, made available to PANA here Friday, disclosed. According to Congolese Health Minister Auguste Mopipi, “the product, sold in the streets of Kinshasa and in some pharmacies in other parts of the country, is dangerous for children and does not heal malaria but rather worsens and complicates the state of patients….The ‘counterfeit’ paediatric quinine was modelled on that of the quinine syrup of 100 ml, manufactured by the Zenuphar firm that denounced the counterfeiting. The analysis of samples of the counterfeit product, made in Kinshasa, at the quality control department of the pharmaceutical firm’s laboratory, stated that “Quinizen 20%” did not meet pharmaceutical standards. The country’s health ministry has set up a commission of inquiry to dismantle the network of manufacturers of the counterfeit product.
Some Intervention Efforts are Underway
Nigeria appears to have had some success battling this public health crisis. Since 2001, the NAFDAC has reported numerous successes and has been credited with reducing the amount of counterfeit drugs on the market. While no formal estimate should be taken uncritically and further research should attempt to confirm the reduction, progress appears to have been made in curtailing Nigeria’s counterfeit drug markets by the NAFDAC’s persistence.
The NAFDAC was established in 1993, but for several years the organization was deemed by some to be unable to control the counterfeit drug epidemic (Bate, 2008b). In 2001, the WHO estimated that 70 percent of the drugs being sold in Nigeria were counterfeit and little was being done to combat the problem (Primo-Carpenter, 2009). In 2002, Nigerian health officials estimated that counterfeits made up 40 percent of the pharmaceutical market (Primo-Carpenter, 2009) and a study cited by the American Council on Science and Health estimated that 85 percent of Nigeria’s malaria drugs were fake or substandard (Yankus, 2006).
Prior to 2001, Nigeria was the main market for counterfeit drugs in sub-Saharan Africa; as a result, neighboring countries responded by banning all pharmaceutical products made in Nigeria (Bate, 2008b). This led to the appointment of Dr. Dora Akunyili as director-general of the NAFDAC.
Akunyili restructured the agency and strengthened import and export security by limiting the importation of all drugs and other regulated products to two seaports and two airports, and banning such imports through all land borders (Bate, 2008b). The NAFDAC was also given the authority to demand that the Nigerian Ports Authority, independent shipping lines, and airlines release all shipping and cargo manifests to agency inspectors (Bate, 2008b). Additionally, a large-scale public education campaign was undertaken to increase public awareness of the counterfeit drug problem. Every two weeks the NAFDAC discussed the differences between counterfeit and genuine drugs in Nigerian newspapers and on radio stations. As a result, between 2001 and 2006, Nigerian officials reportedly identified and destroyed more than US$ 109 million of fake drugs (Edike & Obinwanne, 2006). In 2006, a WHO IMPACT report (citing the NAFDAC) announced that the amount of counterfeit drugs had been reduced to 16 percent of the total drug market in Nigeria (WHO, 2006b).
Recently, the NAFDAC’s new director-general, Dr. Paul Orhii, reported that over the last 8 years more than 120 destruction exercises of counterfeit and substandard drugs have been carried out by the NAFDAC, with 45 counterfeit drug offenders being convicted for their crimes (Obinna, 2009). Orhii also reported that regulatory officers would be trained in the use of new technologies that allow them to test and detect the quality and efficacy of drugs coming into the country. In addition, the NAFDAC will soon partner with the private sector to better organize the country’s pharmaceutical distribution network (Obinna, 2009).
International efforts have been made to curtail criminal attempts to get counterfeit drugs into Africa as well. INTERPOL has been working with numerous police agencies to coordinate operations to track the movement of counterfeit drugs into Africa from other regions of the world. Additionally, in February 2006, the WHO created the first global anti-counterfeiting partnership, the International Medicinal Products Anti-Counterfeiting Taskforce (IMPACT). Together, these efforts have resulted in numerious successes:
- In August 2007, the Chinese pharmaceutical company Holley-Cotec recalled 20,000 doses of the anti-malarial duo-cotecxin from Kenya after testing results revealed low levels of active ingredient (BBC News 2007).
- In September 2008, Belgian authorities confiscated more than two million counterfeit anti-malarials and painkillers that were manufactured in India and were being shipped to Togo for distribution (BBC News, 2008).
- In September and October 2008, INTERPOL led inspections of 191 locations in Tanzania, including pharmacies, warehouses, and illicit markets, resulting in the seizure of more than 100 different types of counterfeit drugs; law enforcement officials closed four pharmacies and 18 drug shops. (INTERPOL, 2008b).
- In September and October 2008, INTERPOL led inspections of 45 pharmacies and drug shop locations, 38 of which were investigated further for operating drug businesses without the required licenses and controls to ensure drug safety genuineness (INTERPOL, 2008b).
- In November 2008, INTERPOL confiscated US$ 6.65 million worth of counterfeit HIV/AIDS, malaria, and tuberculosis drugs in Southeast Asia and made 27 arrests (Kaiser Network, 2008).
In addition to the international and governmental response, private drug companies have stepped in to reduce this illegal trade. In June 2007, European drug companies announced plans to introduce new security measures, including two-dimensional bar codes and tamper-resistance packaging. In 2008, Pfizer held a conference in South Africa at which customs officials, regulators, the WHO, the Pharmaceutical Security Institute, and representatives from 10 sub-Saharan governments came together to discuss the counterfeit drug epidemic in Africa and ways to combat it. Important Unanswered Questions Remain Due to the limited amount of information about illicit drug markets and organized crime and their relationship to the pharmaceutical counterfeiting process, there are many questions that need to be answered before evidence-based policy and intervention strategies can be put into place. Among the actions that could answer some of the most fundamental questions are the following:
- Identify the level and forms of corruption surrounding the counterfeit drug problem, assess its relation to the counterfeiting process, and, if necessary, consider ways to reduce it.
- Identify those who are producing, distributing, and selling counterfeit drugs and analyze their characteristics, levels of organization, and processes.
- Identify the strengths and weaknesses of law enforcement and customs personnel in intercepting and preventing counterfeit drugs from entering their country. Areas of interest might include ports of entry screening procedures, training in forgery and counterfeit document identification, and technology being used to assist in the detection of counterfeit drugs and documents.
- Articulate how counterfeit drugs are distributed once they pass customs and law enforcement personnel.
- Identify and evaluate current drug regulatory controls, quality assurance procedures, and intervention strategies to discover weaknesses and propose ways to strengthen them.
- Identify the ways in which pharmacists, health care providers, and consumers authenticate drugs, and the kind of training that would assist in identifying counterfeits.
- Identify how counterfeit drugs are getting into Africa by investigating the supply chain and the trade routes used by the suppliers and smugglers.
- Evaluate the current punishments and penalties for drug counterfeiters and determine which penalties may best prevent the crime.
- Determine what government authorities are doing to stay current on trends and methods used by counterfeiters.
- Estimate the country-specific quantities and the cost (by type) that counterfeit drugs represent each year.
- Estimate the country-specific quantities and the cost (by type) that counterfeit drugs represent each year.
- Examine the forms and extent of crimes (and their effects and prevention) associated with the counterfeiting process.
- Investigate how and the extent to which the Internet facilitates the trade of counterfeit drugs in Africa.
- Assess potential strategies to reduce the demand for counterfeits.
- Examine ways to reduce the supply of counterfeit drugs by strengthening law enforcement and rule of law institutions.
- Examine the effectiveness of educational programs in reducing the purchase of counterfeit drugs.
- Conduct an international assessment of promising practices for combating pharmaceutical counterfeiting (demand, supply, and process) for use in African countries.
Conclusion
The production of counterfeit drugs has been referred to as the “perfect crime” because a false drug is difficult to detect and the profit for the counterfeiter is high (Kontnik, 2004). Because of the challenges in detection, there is much we do not know; societal, economic, and human costs due to deaths and injuries caused by counterfeit drugs may be higher or lower than what has been estimated. The estimates provided above are based on data collected by international organizations and the countries currently dealing with the counterfeiting problem. Anti-counterfeiting strategies should be evidence-based with a primary focus on understanding and securing the pharmaceutical supply chain from counterfeiters. Any strategy or intervention considered should be supported by objective data and analysis.
2009 Copyright Michigan State University Board of Trustees.
